My past year as an NIH-funded scientist at an R1 institution
I always told myself I’d do this science thing until the stress outweighed the joy. I don’t like stress, so I built that into my career plan. The baffling thing to me is that I became a scientist in the first place. Is it stressful? Yes, and leagues more this past year. But here I am.
To understand why this year forced me to stop and reckon with the work I do, you need to understand what this job actually entails. What does my day-to-day look like? Well, it’s a lot of writing. In addition to overseeing the implementation and timelines of multiple long-term projects and mentoring my team, much of my workday is spent writing manuscripts and new grant applications. In science, writing is the currency that sustains the work. You may have heard the phrase ‘publish or perish’ and its true: without writing (and publishing!) science does not move forward.
An R1 institution is a university classified by its high level of research activity. Here, faculty roles center on securing external grant funding, like those from the NIH, which support large‑scale research programs. In practice, this means that scientists essentially run their own labs like small businesses. We generate the ideas and develop them into long-term projects, typically spanning five years. We seek investors through competitive grant funding, build and manage our budgets, and use those grant dollars to pay our own salaries along with those of our lab technicians, graduate students (and their tuition!), and postdoctoral fellows. We hire, we fire, and we are responsible for ensuring these complex projects are carried out in a timely, and ideally groundbreaking manner.
All of this is done through multi-million dollar grant contracts with the federal government. What is less visible to those outside the system, is that these contracts are often awarded in a deficit. NIH project grants are routinely cut but 10-20% from the proposed budget, with little ability to reduce the scope of work (believe me, we’ve tried!). In recent cycles, I’ve seen some cuts approach 25%, yet investigators are still expected to deliver the same proposed science, often by absorbing the shortfall through efficiency, unpaid labor, or institutional support.
You may have heard about the ‘high rate’ of indirect costs on NIH grants. Some institutions will allow researchers to use a portion of these funds to help cover funding gaps, including these NIH budget cuts. In most other cases, those indirect costs go back to the university to build and maintain laboratories, oversee health and safety regulations, maintain data security and research compliance, and to keep the lights on. For better or worse, the NIH indirect cost structure was intentionally hard-wired into the system to build the United States research infrastructure to what it is today, until recently: the envy of the world. But without these grants, none of us get paid, the labs don’t get used, and the lights go out. Not just for individual labs like mine, but for the entire national research infrastructure that we, as taxpayers, have built over the past 75 years.
Provisional by design
It’s funny. When I tell people that I’m a professor, their first question is usually what do you teach? The truth is, I teach how to be a scientist. At a medical school and R1 institution, I do not have any formal obligation to teach courses. That said, education is a pillar for an academic promotion, and is therefore expected. This can take the form of mentoring my team, organizing a seminar series, or giving invited talks. One of the more intensive faculty options would be to lead full graduate‑level courses, which involve designing syllabi and coordinating expert faculty to teach individual topics, though few of us will develop and teach courses like the ones you remember from undergrad. While this teaching is expected for promotion, it is not what sustains our positions.
Our jobs as medical school research scientists rely on grant funding to pay most or all of our salaries. There is no tenure-based stability. No grants means no jobs. Mine included. Even after decades of high-level productivity and excellence, I am always provisional.
The consequences of this funding structure are not abstract. At any given time, I am not leading just one project, but two or three multi-year, multi-million dollar efforts that collectively support myself and my team, while also working on applications to fund two or three more. I take the support, eduction, and training of my team very seriously. Each week, this accounts for hours of mentoring: working through experiments and concepts, helping them revise their writing, and generally training them to become rigorous, creative scientists. When trainees secure their own grant funding through NIH- or foundation-supported training grants, it is a huge relief. One of my biggest stresses is that a lapse in my grant funding could mean failing the people who depend on me for not only their training, but their livelihood.
When the grants run dry
So far, in fiscal year 2026, (beginning October 2025), new grant funding levels are down 63% from prior years before this chaos began. This striking difference is shown in this graphic from the Washington Post. The Association of American Medical Colleges has great info on this as well. NIH is on track to have the lowest funding rate in decades.
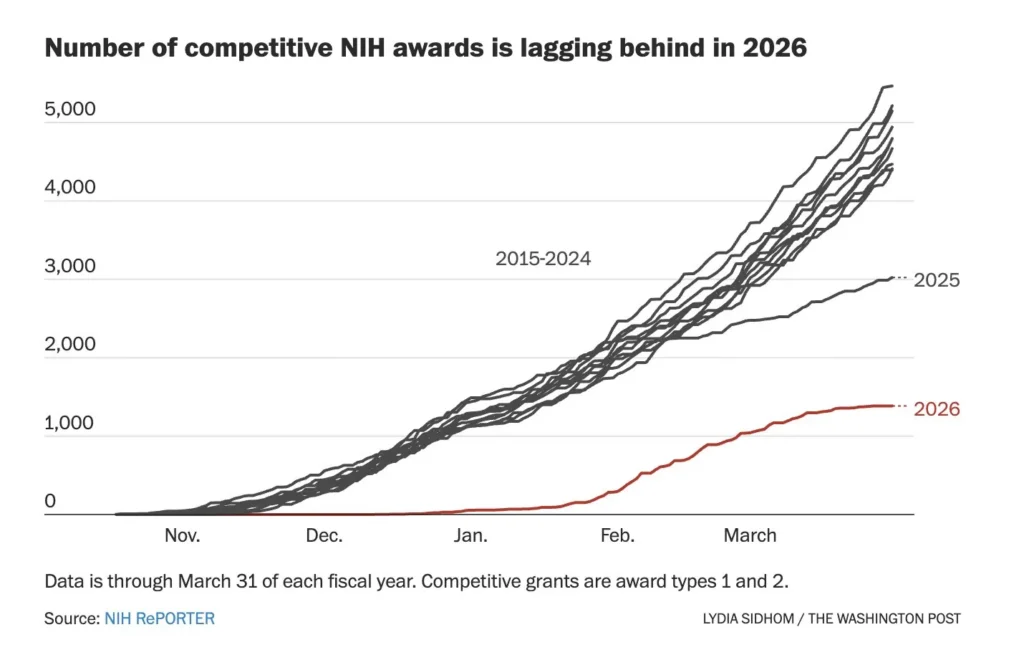
To further put this in perspective, the NIH budget typically represents less than 1% of total federal spending, and just 2.6% of total expenditures at the Department of Health and Human Services. NIH funding also carries over 2.5‑fold return on investment. We could even argue that NIH funding should be far higher, given the human health and economic benefits. But the numbers alone make one thing abundantly clear: this isn’t about saving money. It’s about breaking the system.
Some of this slowdown reflects delays in grant review during the government shut down, which are only now getting underway. But drastic cuts to administrative staff that oversee and implement disbursement, new layers of political oversight, and delays tied to shifting funding priorities have all compounded the damage. Bear in mind, it is Congress that mandates NIH funding priorities through budget appropriations. Congress allocates spending and creates legal mandates for funding in specific research areas, like they have for women’s health, cancer, and precision medicine. With the most recent budget passed in January 2026, Congress reaffirmed NIH’s funding priorities and made clear that the agency must administer awards without disruption. And yet here we are.
Now imagine if you ran your small business this way. Drastic, unanticipated cuts. Long delays in decision‑making, for months or even years. Excellent ideas left on the table. Imagine letting long‑time employees go, along with years of specialized training, simply because of these delays. Despite money being available and required by law to be spent. That’s not fiscal responsibility. It’s dysfunction.
“this isn’t about saving money. It’s about breaking the system.”
What has this looked like for my lab and me personally? First, money has always been one of my biggest stressors, personally and professionally. And this is clearly a financially stressful time. One application I submitted in October 2024 scored very favorably. Well within typical funding range. But after months of delays, as another five-year grant ended and that new funding failed to materialize, I had make the difficult decision to let a long-time employee go. There were simply no good options left.
One of the hardest parts has been not been the loss itself. It has been holding hope for my team, while carrying my own fears. Everyone in my lab is still early in their training. They are building skills and preparing for futures that depend on the stability of the system they are training within. At the same time I have to be realistic and careful to hold space for their anxiety about training into a system that may not be here in five years. Balancing reassurance with realism and encouragement with transparency is a difficult needle to thread.
This uncertainty is made harder when you consider just how competitive NIH funding is. NIH funding rates typically cover about the top 10%, and a smidge higher for early-career investigators. Proposals are evaluated by top experts in the relevant scientific area and are scored not only on scientific rigor and innovation, but also on their potential impact for improving human health. Even on a good day, this process from submission to award disbursement takes nine months or more. Bear in mind, this is competition among the best researchers in the field. Many investigators submit ten or even twenty applications for every one that is ultimately funded, and many never receive funding at all. Achieving sustained funding year after year is extremely difficult. And now, even grants scoring well within the top 10%, projects that could help so many people, remain unfunded. What feels most destabilizing is not rejection itself, I’ve had plenty of that, but that the outcomes are no longer governed by a transparent or consistent process.
But to be honest, I consider myself lucky. I have seen labs shutter this year. I am much more established and when this started I had several large projects funded to carry me through this past year. I could not even imagine being a new professor just setting up their first lab at this time. This is such a difficult place for a new scientist to be. Delays like those we’re experiencing can make or break a new lab. I want to hold hope that we can get through this and come out better in the end, but with full understanding that, were I in the same place, I may not have made it through uncertainty like this.
Who gets to stay
Layered onto this uncertainty for project funding is the training of the next generation of scientists. I am the Associate Director of a postdoctoral training program in Nutrition research that has had continuous support from the NIH for over 35 years. That continuity has allowed us to train generations of scientists to be thoughtful, rigorous, and responsible Nutrition researchers. We have just received one of our strongest scores in the program’s history. While we remain hopeful that funding will be awarded before the next cohort begins in July, for the first time we are uncertain. Without that funding, we simply cannot support the new fellows or maintain the training environment we have spent decades building.
“One of the hardest parts has been not been the loss itself. It has been holding hope for others, while carrying my own fears.”
This uncertainty around training also raises questions about who is able to persist in this environment. I did not grow up wealthy, or in academia. I am a former WIC-kid, Pell grant recipient, and first-generation college graduate. My passion for science is what brought me here, not my background. I myself was supported and trained by this same program when I was fresh out of graduate school. That early support gave me a foothold in Nutrition research and allowed me the time, mentorship, and intellectual freedom to develop to the scientist I am today. Without it, I would not be here.
By NIH metrics, my background places me squarely within the categories of trainees supported through diversity‑focused funding mechanisms. Many of which have been targeted or destabilized in recent cycles. It is people with backgrounds like mine who are most vulnerable to these funding delays and cuts. Passionate, brilliant scientists who may never get a foothold in this competitive environment, or who may struggle to stay when the objective ‘best of the best’ is no longer enough to pay the bills.
While I did not grow up in academia, I did grow up a child of a small business owner. Of a whole family of them, in fact. I’ve seen businesses succeed and thrive, and I’ve watched them fail. That perspective shapes how I see what is happening now. What this funding uncertainty is doing to our ‘small‑business labs’ is a recipe for failure, and not only for researchers. It is a profound waste of public investment: projects half-completed, millions of dollars spent only to be shuttered before meaningful outcomes can be achieved, students half-trained, clinical trials stalled. All of this on top the last seventy-five years of public funding that built the research infrastructure we now risk dismantling.
“Passionate, brilliant scientists may never get a foothold in this competitive environment, or may struggle to stay when the objective best is no longer enough to pay the bills”
I consider it my utmost responsibility to spend your tax-dollars wisely. I take your investment seriously and only hope that the work do I returns value in the form of better health, deeper understanding, and knowledge that others can build on. This commitment is part of why the past year has been so destabilizing to me personally. Since late January 2025, I’ve been forced to have a reckoning with my life choices. Have I reached that tipping point where the stress finally outweighs the joy? Am I still on the right path? I lost about ten pounds last February (I’m a stress ‘can’t eater’). I found myself wondering how to bring my love of science to the world when it is being so senselessly attacked, or if I even should.
I remember I had a similar life-reckoning in graduate school. They say your 29th year is a doozy and mine was no joke. I questioned every life decision I had ever made to that point. I took a month-long backpacking trip through Spain and Morocco to step outside of the science. To gain a broader perspective of the world and my place in it. I drew beautiful pictures of the Mosque in Córdoba (or tried to). I ate freshly picked dates and fell asleep under the stars in the Sahara. That trip took months of planning and every penny I had, but boy did I need it. By my birthday that year I could tangibly feel my love for my science returning. The passion for my work that got me out of bed every morning, excited to go to the lab.
This love is extremely important in science. We routinely tell our students when choosing a project or lab to find one that you love. It is so difficult to succeed without this love because science is incredibly hard and riddled with failure: Experiments fail, papers get rejected, grant applications do not get funded. If you don’t love it, I’m not sure why you’d keep going. For me, I’ve done fairly well. Since my postdoc started in 2009, I’ve never had a lapse in NIH funding. I’ve had consistent support and buy-in from organizations like The Obesity Society and the American Diabetes Association. It was never easy, but it felt manageable.
Some days, I find myself asking whether it’s selfish to keep doing science on your taxpayer dime. What gives me the right to love my job so much? Other days I know the answer. Though this work is slow: it takes years, sometimes decades, to find the answers, I know that it does matter. I am making a difference. I’ve developed tools, ideas, and knowledge that others now use to advance their own research. That’s how science is supposed to work.
I stay because my love of science still gets me up every morning. I still love writing grants. And now, I also love writing pieces like this, hoping to pass along some of this love to you. Maybe it sounds trite, but I fully believe that knowledge, truth, and science will get us through this difficult time in our history.
I stay because of the people, the wonderful, dedicated colleagues I work alongside and the brilliant scientists I’ve had the privilege to help train. Watching nascent scientists grow into creative, capable colleagues is one of the most meaningful parts of this job. People who are working hard every day at the slim chance their efforts might improve our collective health. More than myself, I speak out for them.
Last week I started writing a new NIH grant application. For the first time since January 2025. I’ve submitted applications to other organizations and lightly revised NIH proposals in the meantime, but returning to the deep work of a new application reminds me why I’m still here. I don’t think my longevity in this field is because I tolerate stress well at all. I’m beginning to think it’s because I just love the science that much. Where else could I dream up my wildest ideas for solving incredibly complex health problems and be paid to pursue them? I can appreciate that not everyone is as excited about science as I am. But the truth is, this work excites the hell out of me, and maybe that is why I keep choosing it.
